By the time I started MedSchool, I haven’t seen a lot of hospital movies or series. But with time, the curiosity grew, and I finally decided to find out what is presented to the larger public as a “doctor”. I watched Dr. House, Grey’s Anatomy and Scrubs as a start.
Inspired by the series and movies, it isn’t much of a coincidence that my first clerkship was at the Department of Trauma Surgery – and not very surprisingly it turned out to be very different than anything TV had ever shown.
Most differences are more or less obvious: There is no insanely deep talk about relationships during surgeries, people do not storm out dramatically or make big scenes to make a point, ORs are kept sterile, doctors do what they are specialized in and do not make extremely hard diagnoses within 10 seconds.
On the other hand, there are similarities: It is pretty hard for assistant doctors (residents and fellows) to get to do surgeries and you have to find a senior doctor who likes you and will push you. There is a common room for OR staff, but it is not for making out: people just eat there and chill in between surgeries. Also, hierarchy is a thing and the senior surgeon chooses the music, but it isn’t a must to listen to music.
Here are 4 things that I found crucial or were new to me during my clerkship at the Department of Trauma Surgery.
1 – It’s the anaesthesiologists that keep you alive.
Operations are probably on top of the list of what TV portrays wrong, starting with the obvious lack of sterile environment in TV-Operations.
What startled me more is that in many series and movies, it seems like the surgeons look at the famous screen with vitals like blood pressure, heart rate etc. at every step of the surgery and then when something goes wrong they say something like: “They’re crashing. Push five of epi!”The truth is that in most cases surgeons do not even see the screen with all vitals and they are not in charge of checking on the patient. While operating, the surgeon focuses on the operation only, once in a while they would check with the anaesthesiologist on how the patient is doing.There is a reason why intensive care and anaesthesiology are one specialty in Austria and other countries.
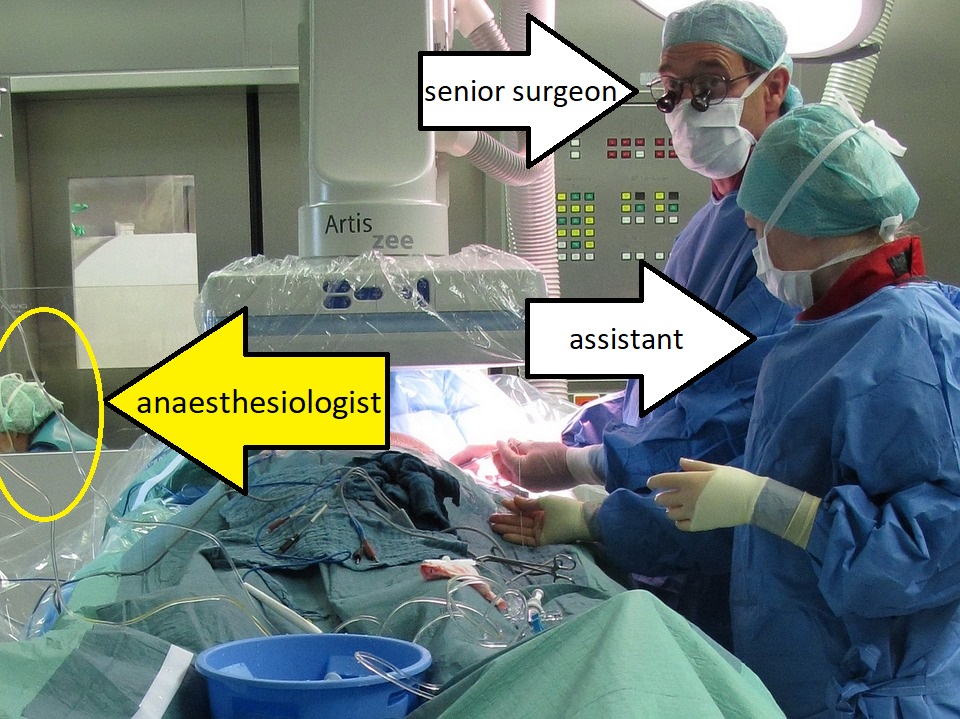
The standard surgery would look something like this: Before your surgery you’ll get a visit from an anaesthesiologist who will check your vitals and take some measurements, based on which they will calculate what kind of anaesthesia you will get. Then, when the OR is ready, you will be brought to the preoperative area, where the anaesthesiologists will start the preoperative measures. Depending on what kind of surgery it is, there are different preparations involving things like intubation, ECG-screening, placing of a central venous line, checking vitals etc. At this point, the assistant surgeon may have arrived. The next stage is placing the patient on the OR table, which is dependent on the patient’s wellbeing. I’ve seen patients where it took only an assistant doctor and two OR nurses to position the patient, when in good health. Patients that are in intensive care will be positioned by experienced ICU/anaesthesiology nurses and doctors with help from the others.
After a really tough operation, the patient lost pulse and an ICU/anaesthesiology nurse was sitting on the patient’s bed doing chest compressions (very Grey’s Anatomy-like), while the anaesthesiologist was giving orders (this was actually a “push five of epi”-situation). This scene I cannot get out of my head: when the main surgeon left and the assistant as well – there was this team of anaesthesiologist and their nurses trying to save that patient’s life. I was in there too – the last one from the trauma surgery department – just trying to help where I could: holding cables and drainages or getting a blanket. The crash team was ready to defibrillate, they were counting down 2 minutes while the nurse was switching with a doctor again to do chest compressions and just as the crash team said two minutes are over, the main doctor said “I have a pulse”. All of it seemed very unreal, very movie-like – only that the team doing their best to keep that person alive were the anaesthesiologist. The surgeons had long gone, taking care of another polytrauma that had come in, trying to save that person’s legs, or spine, and life with the help of another anaesthesiology team.
This leads to the second point:
2- You do one thing, and one thing only
There is a reason medical staff specializes in different fields– not only doctors but also nurses can specialize in certain departments. Criticism of specialisation leading to doctors being blind to a general perception of the patient is legitimate, but the solution in my opinion does not lie in doctors doing everything but in doctors being taught to communicate with each other and departments working together and lots of other things, but this is a different topic.In series like Doctor House or Grey’s Anatomy, it seems like doctors do all of the work: admit the patient, draw blood, run tests in the lab, push them in their beds around the hospital to do x-rays or CTs, diagnose the images, make out in on-call rooms. Here are some things that you do as a surgeon:
– Physical examination
– Operate
– Plaster casts
– Rounds
– Read lab results (from the lab department)
– Look at X-Rays
– Look at CTs and MRIs (+ read the report from the radiologist)
– Draw blood and venous lines (in some wards done by nurses, students)
– A lot of mending minor injuries in ambulance
– Diagnose after doing most of the above
List of things you do not do as surgeon:
– Anything that would require you to specialise in another field as for example Medical and Chemical Laboratory Diagnostics or Radiology
3 – Talking during operations
As mentioned earlier/above, the OR staff does not talk about very personal and irritating affairs during an operation. Mostly it is small talk. Sometimes the senior doctors would explain details of the operation to the assistant doctor or students and answer questions. Sometimes, when I was assisting, they would question me about the operation to see how well I was prepared. Often there would be silence that was only broken when the operating doctor asked for instruments or lights or to ask the anaesthesiologist how the patient was doing.But of course there were some trivial things as well: Discussing patients with interesting tattoos (is it a neo-Nazi sign or not?), friendly disputes between a German nurse and an Austrian doctor on how to say potato (Erdäpfel – Kartoffel) or annoyed comments about the neurosurgeons for blocking the OR.I know it doesn’t make for a good series to have a professional environment during operations, but I feel like there is a middle ground between very over-the-top fights and boring conversations.
4 – There is no deep life lesson at the end of the day
This one is very simple: There is no voice-over that concludes the day and makes you realise what the cases you had that day were supposed to teach you because, coincidentally, they all summed up in this big life lesson. Working in a field that has to do with sick people, their relatives and what system we put in place to treat them, confronts you with a reflection of humanity and society every day. I learned a lot regarding communication, dealing with death and empathy. Sometimes it is a quiet day, sometimes it is a stressful day, and sometimes patients die. The day ends and you have to be able to go home and leave it behind.
There are no constant very emotional “real-talks” with huge plot twists. After two weeks I felt that I was still learning but the days repeated themselves. There is no sudden realisation that it all has a purpose. Things happen, you fix them, try to give advice on how to prevent them and reach the best outcome.
I remember the one case that I struggled the most with, was a homeless person that would show up once in a while. He had cut his hand and what would be a very easy wound to fix (cleaning and a few stitches), turned out to be a threat to his life. He wouldn’t show up for follow-ups, his bandage would get wet and the wound and sutures would infect. I was working the night shift, when he turned up again and his wound looked horrible. I asked the doctor whether we could try to contact someone or if we could put him in rehab, as he was clearly drunk every time. He denied as the patient had refused to say anything on relatives or give out any useful information. And to be admitted to rehab, one must do it by their own choice and we couldn’t do more than offer him help. I asked him what would happen if he kept coming unregularly and the wound infected. The doctor said: Maybe he will die from a sepsis or we will have to amputate his arm if he shows up on time. At first it sounded very apathetic and rude and I felt very angry. But with time, I realised that there was nothing more he or I could do, things like this happen and you have to know your responsibilities and boundaries if you want to survive in the medical field. You have to accept that there are people who ask for your help when you reached your limit and cannot help them anymore and that there are people who will refuse your help while you know that treating them could save their life. This is something they teach at MedSchool but it is another thing to experience it first hand with a real patient.
This may be the closest thing to a life-lesson I experienced at the hospital. To end this on a positive note: Before I left I saw the homeless patient in the waiting room – on time for his follow-up. Also: long live the universal health care system in Austria.
Disclaimer: This article falls out of the usual essays I write as it is based on my experience at the Department of Trauma Surgery in an Austrian hospital rather than science. The procedures described above might differ to other hospitals and countries.
Thanks to Birgit Jorda for editing.


Gut geschriebener Text Marina weiter so